In most traditional health care settings, private parties involved tend to function within their domain of expertise strictly. However, with the increasing health care demands, cost associated and efficiency that is necessary to maintain a higher value of quality of attention with low costs, it is becoming apparent to the necessity to have much closer collaborations, i.e. convergence between different themes, domains, and industries[1-3]. An editorial by Byron C. Scott defines convergence in health care as follows: “1. The collaboration of payers and providers (physicians and hospitals) to provide population health management, and 2. Divergent health care organizations were becoming similar organizations” [2]. Perhaps, this definition may be extrapolated to preventive health care, where ‘the convergence of preventive health care can be defined as the collaborations between general public, patients, health care providers, financial and economic analysts, funding agencies, marketing, management, life sciences companies, pharmaceutical companies, policy makers, biomedical communications, and researchers are established, managed and improved in order to achieve the primary goals of preventive health care and provide efficient health care services with reduced cost (Figure 1)’. Individual health care professionals working towards this goal refer to this concept as ‘Enlightened Health care Ecosystem’ [1,4].
Figure 1. Convergence of Medicine
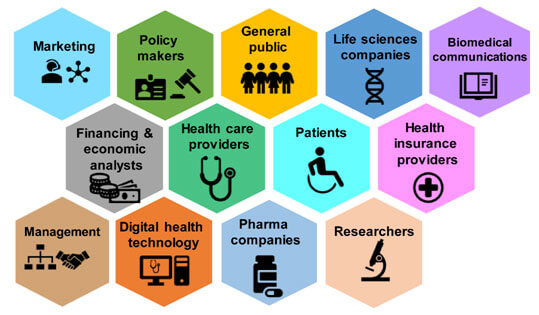
The convergence in preventive health care is not a novel concept, but rather a long-lasting concept that needs to be updated and modified based on today’s health care demands. Some of the oldest reports on convergence in medicine come from studies that integrated skills and resources available for individualized/personalized health care and community-based/population-oriented health care [5], and integration of occupational health psychology with public health and preventive medicine[6]. Even though these examples come from the 1990s, the central emerging concept is the integration of different domains or dimensions of medicine under one controlled organizational setting to achieve the goals of preventive health care, namely, preservation of health, restoration of impairments, minimization of distress and finally, prevention of death [7].
| Recommended for you | |
| Preventive medicine is the solution and vision for future | |
| 4 Digital health technologies in preventive health care | |
| 13 Themes of preventive medicine |
Figure 2. Preventive health care themes
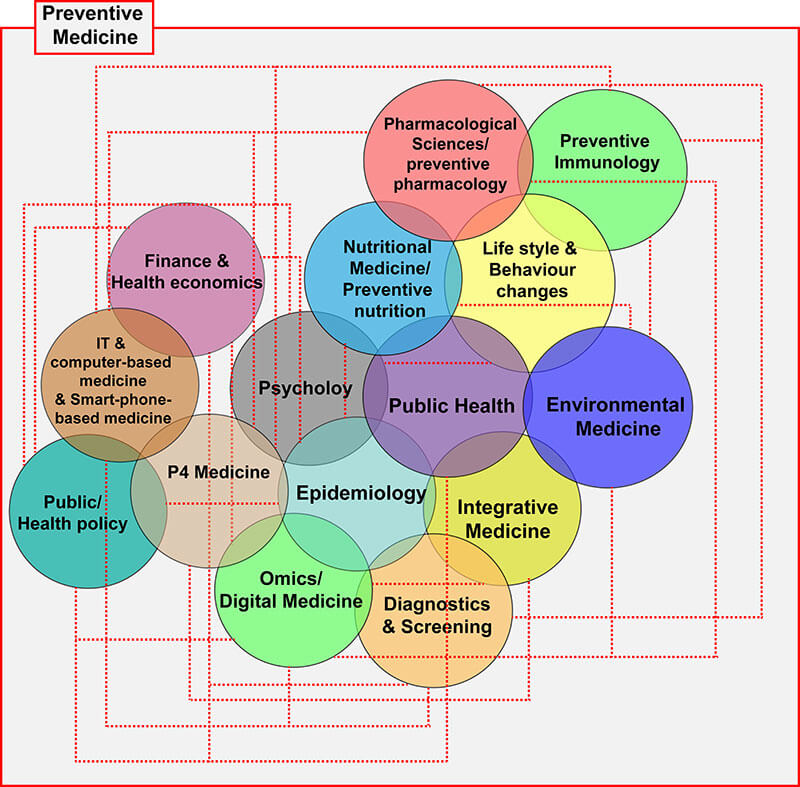
Different ideas that come under preventive health care seldom function in isolation (Figure 2). As the figure itself speaks, each issue is overlapping with several others. It can be expected that as each theme develops by its own and it relates to other subjects, the convergence between them become more apparent and the borders may start to disappear, creating a multifunctional unit or health care ecosystem.
Integrative medicine
Integrative medicine is a fast-growing framework which connects many of the themes of preventive health care [8] (Figure 2), namely P4 medicine framework, omics and digital medicine, diagnostic screening, epidemiology, public health and environmental medicine to say the least. One example of integrative medicine where two or more domains have converged to attain health promotion, disease prevention, and health protection is Public health and Preventive Medicine (PhPm) [9].
Convergence of conventional medicine with complementary and alternative medicine (CAM)
The health care professionals who practice traditional Western medicine are beginning to realization and appreciation of the advantages of combining conventional medicine with CAM approaches which involve mind, body and spiritual healing and the use of natural non-pharmaceutical substances[10]. This convergence modifies the general biomedical model of health care. CAM gives much priority to psychology and mental health. As illustrated in Figure 2, psychological aspects of preventive health care have avenues that overlap with P4 medicine, epidemiology[11], public health[12], nutrition[13], lifestyle and behavioral changes[14], pharmacology[15], and health policy making [16]. Integration of the expertise of psychologists, psychiatrists, and social workers may indeed promote the development of health care at individual, institutional levels as well as population levels [17].
Skill mix in health care
Whether in emergency care or non-urgent primary health care, the team structure and the skills of health care professionals involved are extremely critical to delivering proper preventive health care. Several recent studies highlight the importance of having a skill mix and properly trained team dynamics in favorable clinical outcomes [18,19] and organizational outcomes[20]. It is their recommendation to have doctors, nurse practitioners, registered nurses, clinicians [19,20], support workers, administrators, allied professionals, professional human resource management and laboratory technical staff[20]. Moreover, they recommend having multiple disciplines of health care professionals which have been shown to increase patient outcomes [21]. For instance, having a multidisciplinary primary care team practitioners, social service staff, community workers, volunteers, and pharmacists was shown to improve better primary health care delivery [20,22]. This evidence also supports the convergence of health care domains to achieve the goals of preventive health care.
Image credit: www.istockphoto.com

















