New definition of digital preventive health care
We come across the phrases ‘digital health’, ‘digital medicine’, ‘digital prevention’, and so on when digital technologies are used in different branches of healthcare. The term ‘digital prevention’ has surfaced recently and has been interpreted in many ways. The confusions and misleads have urged us to further look into how digital health coincides with the ‘preventive health care’.
The literal meaning of prevention or preventive healthcare is the prevention of disease occurrence, eradication, elimination or minimizing the negative impact of the disease and ultimately prevention of death. Therefore, preventive health care does not simply involve prevention of diseases. This shift in our perspective of preventive healthcare should, therefore, be applied to re-defining ‘Digital Preventive Healthcare (DPH)’ or ‘digital prevention’.
“Digital preventive healthcare is defined as the use of digital health technologies in prevention of disease occurrence, eradication, elimination or minimizing the negative impact of the disease and ultimately prevention of death.”
If the levels of preventive healthcare proposed by (Leavell & Clark, 1953) are applied to the novel perspective of digital preventive healthcare, further categorization of digital preventive healthcare emerges that also aligns with the progression of a disease. The levels of preventive health care are primordial prevention (level 0), primary prevention (level I), secondary prevention (level II), tertiary prevention (level III) and quaternary prevention (level IV). As such, the DPH is also categorized into five levels as, DPH-0, DPH-I, DPH-II, DPH-III, and DPH-IV.

When DPH prevents death… Old definitions merge, and new definitions emerge
Depending on the disease condition and preventive healthcare approach employed, the classification provided in Figure 1 may show some overlap. One such situation is the prevention of depression-associated suicide. Some may not consider depression and its deathly consequences (i.e., suicide) as a ‘true disease’ in contrast to cancer or diabetes. Yet, such perspectives cannot undermine the severity of this public health issue.
According to the projections by World Health Organization (WHO), more than 1.5 Million suicides are anticipated by 2020 (Bertolote & Fleischmann, 2002), and that demands attention and methods of prevention!
Regardless of where this health concern fit into the DPH categorization, current technological advances have made significant improvements to prevent death by depression-associated suicide.
Digital prevention of death by suicide involves mHealth such as smartphone apps and wearable sensors, gamification concepts in digital gaming, big data applications and cloud machine learning and remote monitoring.
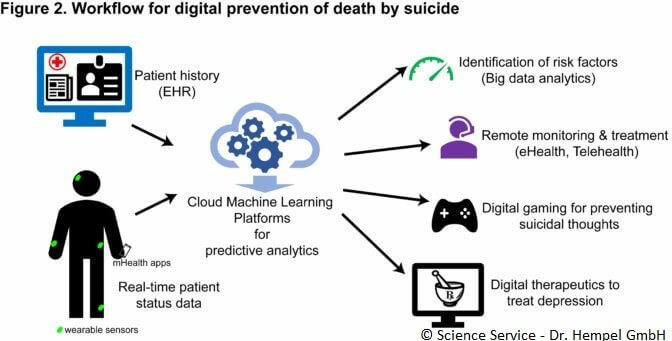
Electronic health records provide the patient history of any mental health conditions and suicidal attempts that are quite useful in the digital prevention of suicide. The novel wearable sensory devices that record electroencephalograms (EEG) and wearable biosensors that are connected to smartphone apps have been employed in implementing could-based monitoring systems for tracking mental state (Alam, Cho, Huh, & Hong, 2014).
These devices are capable of providing real-time patient data. Evidence-based Smartphone apps such as “Mood-Tools–Depression Aid” are available now which can track suicidal or deliberate self-harm (Larsen, Nicholas, & Christensen, 2016).
Cloud machine learning platforms are designed to gather all electronic data from EHRs, and mHealth devices and perform predictive analytics to identify risk factors for suicide, make predictions on patient’s mental health status, and connect to appropriate digital preventive healthcare channels to make decisions regarding treatment protocol (Vahabzadeh, Sahin, & Kalali, 2016). Then, the patient can either be monitored remotely through telemedicine applications, digital gaming methods are used to prevent suicidal thoughts or patterns, and digital therapeutics are used to pharmacologically-treatable symptoms of pre-suicidal conditions.
‘Digital Preventive Therapeutics’ – it is a branch of digital preventive healthcare in which therapeutic healing and pharmacological applications are employed. In digital prevention of death by suicide, digital therapeutics can be used to treat mental health conditions such as depression that lead to suicide.
Definitions of DPH are distinct and clear when it comes to direct digital disease prevention programs. One such example is the Digital Diabetic Prevention Program (DDPP) which has already been clinically approved and uses the concepts of digital therapeutics (Sepah, Jiang, Ellis, McDermott, & Peters, 2017).
Regardless of the clarity of the definition of each DPH level, it is becoming evident that the digital health technologies can be employed at every stage of disease and to prevent the occurrence of disease, reduction of disability and impairments by the disease and prevention of death. In simple words, DPH is capable of meeting all the basic requirement of healthcare, namely, preserve health, restore impairments, minimize distress and prevent death.
Image credit: www.istockphoto.com

















