The Rich-Poor digital divide in health care and 4 ways to bridge it
Digital equality
Being in a highly revolutionizing digital era, digital technologies that are linked to the internet, smart phones, tablets, etc. (…the list goes on) have become an essential component of our daily lives. As of 2017, there are 3578 million internet users around the globe with a 3.39 billion increase from 2016. Here ‘internet users’ are defined based on their access to through any device. However, looking at the percentage internet users in different countries (Table 1), the stage of development, financial and political stability seems to be a factor that contributes to the capacity to use digital technologies. It has become very evident of the presence of rich-poor digital inequality or digital divide, even within highly developed countries such as the USA. In fact, USA is one of the most prominent example countries where digital divide has created discrimination. Computer literacy, the level of education, confidence or willingness to use digital tools, access to digital technologies, quality of available digital technologies and costs associated with digital technologies are only a fraction of the factors that influence the digital equality.
| Table 1. Percentage of internet users | ||
|---|---|---|
| Country | Internet usage | Ref |
| Germany (2016) | 88% | [1] |
| USA (2015) | 74.5% | [2] |
| Canada (2016) | 88.5% | [3] |
| Ghana (2016) | 28.4 % | [4] |
| Bangladesh (2016) | 13.2% | [5] |
‘The richer you are, the better your health’ – digital discrimination in health care
Current primary health care model has become transformed into highly digitalized systems. Many of the healthcare institutions, associated stakeholders, and patients are heavily dependent on the use of digital preventive healthcare tools such as eHealth, mHealth, and telehealth. While many of the public can access to basic digital health facilities, most advanced and efficient tools involve the use of internet daily, wearables, devices with health applications. These digital preventive healthcare devices can be considered as ‘out-of-pocket’ costs that might only be affordable to the wealthy. That might be one of the reasons for poor people in one of the most developed countries in the world as the USA was reported to have poor health in contrast to the affluent community. In fact, USA has the most prominent income-related differences in health, as reported in a survey from 32 countries [9]. Coverage of digital preventive measures by insurance could be another factor that makes low income-patients not to have access to such treatments, as many of the devices or services may not be covered by insurance. Therefore, for the digital preventive healthcare strategies to be effective, the digital division between wealthy and poor should be bridged, and equal access to all health benefits (including digital health tools) should be provided to all citizens . Not everyone is privileged to have proper education and computer literacy that is required for using digital preventive healthcare tools, to understand the significance of using such services and to have the confidence to use these services [9].
| Recommended for you | |
| Preventive health care is the solution and vision for the future | |
| 10 Digital health technologies empowering patients | |
| Top digital health events in India |
Ways to bridge the digital divide in healthcare
1. Prevention is the key
Preventive healthcare practices aim to prevent the occurrence and spread of diseases. Enforcement of preventive health care, specifically in low-income communities would immensely reduce the incidences of disease occurrence and thereby reduce the health concerns of such low-income communities. Therefore, more resources should be allocated to establish and enforce preventive health care measures.
2. Knowledge is power
Education and training programs to improve computer literacy is one of the major steps towards bridging the digital divide between wealthy and poor. As a step towards this goal, National Health Service (NHS) has launched 5000 learning centers equipped with a computer and medical technology tutors, along with 16 flagship projects designed for patients in rural areas or less access to digital tools [10]. These educational programs may reduce the social gradient in health.
3. Enforcing digital inclusion in low-income communities
The Institute of Museum and Library Services in their Building Digitally Inclusive Communities publication defines digital inclusion as “the ability of individuals and groups to access and use information and communication technologies. Digital inclusion encompasses not only access to the Internet but also the availability of hardware and software; relevant content and services; and training for the digital literacy skills required for efficient use of information and communication technologies”[11]. If the private sector is willing to develop methods enforce digital inclusion through providing Wi-Fi, high-speed internet access, computers/laptops/smartphones with internet connections and wearable medical devices at a lower and affordable cost for low-income families, it is possible to encourage the poor to use digital preventive healthcare tools. The USA has addressed this concern to some extent by establishing the ConnectHome initiative which is a collaborative effort of the private sector, the federal government and low-income communities to have high speed and quality access to the internet[12]. The federal government has further supported ‘digital health inclusion’ of low-income families through the Affordable Care Act and the expansion of Medicaid which provides insurance coverage for these communities[13].
4. Enhancing community healthcare facilities with digital preventive healthcare tools
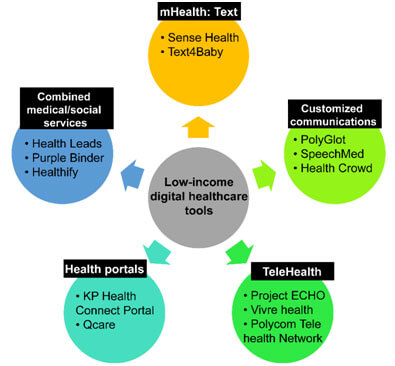 Many low-income families and minority groups depend on community health services for their health concerns as these community services provide more affordable services. The enhancement of digital preventive healthcare technologies in community healthcare facilities that mainly target low-income and minority groups is another way to bridge the digital gap. The Affordable Care Act and the expansion of Medicaid have also supported the use of digital preventive healthcare technologies in community health clinics that majorly provide healthcare for low-income families and minorities [13]. A report by the California HealthCare Foundation indicated several low-cost digital healthcare tools that have been introduced to low-income communities that included mHealth, eHealth and Telehealth tools (Figure 1). The Community Health and Outpatient Care (CHOC) program has now established electronic health record systems and certain other digital technologies that enable coordinated care in 333 outpatient and community health centers[14].
Many low-income families and minority groups depend on community health services for their health concerns as these community services provide more affordable services. The enhancement of digital preventive healthcare technologies in community healthcare facilities that mainly target low-income and minority groups is another way to bridge the digital gap. The Affordable Care Act and the expansion of Medicaid have also supported the use of digital preventive healthcare technologies in community health clinics that majorly provide healthcare for low-income families and minorities [13]. A report by the California HealthCare Foundation indicated several low-cost digital healthcare tools that have been introduced to low-income communities that included mHealth, eHealth and Telehealth tools (Figure 1). The Community Health and Outpatient Care (CHOC) program has now established electronic health record systems and certain other digital technologies that enable coordinated care in 333 outpatient and community health centers[14].

















